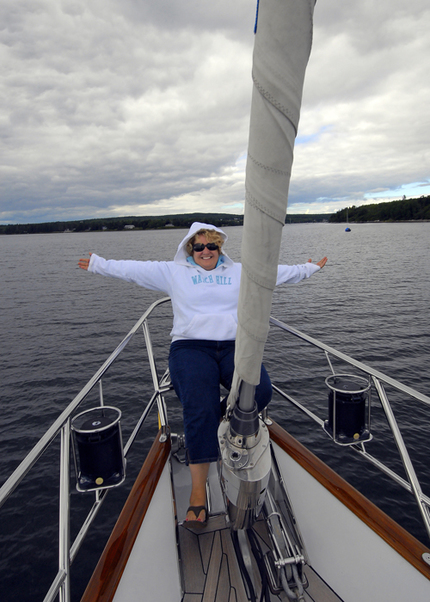 On my brother’s yacht as I begin my final journey
On my brother’s yacht as I begin my final journey In July of 2013, out of the blue, I started to have panic attacks. The first one happened at five in the morning, and John called our neighbor Alicia Powell, a psychiatrist, who came over to comfort me.
The only other time I had a panic attack was when Len had his stroke. That experience lasted for a few days. I just felt waves of fear that were so intense I almost fainted from them.
But these panic attacks were different. They made me feel scared, nauseous, and illogically worried about money and housing.
John recognized the panic attacks as a crisis of faith: being caught between my family legacy of fear and money and the new spiritual world I was birthing. But I knew there was something else also going on, something biological. Sometimes it felt like a dark evil figure attacking me, telling me I should die. I thought I was losing my mind.
To calm myself, I would walk over to Jamaica Pond, lie under one of the maple trees, and breathe in mindful meditation.
The only other time I had a panic attack was when Len had his stroke. That experience lasted for a few days. I just felt waves of fear that were so intense I almost fainted from them.
But these panic attacks were different. They made me feel scared, nauseous, and illogically worried about money and housing.
John recognized the panic attacks as a crisis of faith: being caught between my family legacy of fear and money and the new spiritual world I was birthing. But I knew there was something else also going on, something biological. Sometimes it felt like a dark evil figure attacking me, telling me I should die. I thought I was losing my mind.
To calm myself, I would walk over to Jamaica Pond, lie under one of the maple trees, and breathe in mindful meditation.
By early August I realized I needed professional help, but when I finally found someone my insurance plan would cover they turned out to be on vacation for the month! It reminded me of a movie I saw years earlier called What About Bob? with Bill Murray. His character is so distressed that his shrink is gone for a month that he follows him by bus with his pet goldfish sloshing around in a bowl. It’s a very funny story about how the therapist’s family adopts Bob and his fish while the therapist holds on to his professional boundaries.
Anyway, I finally found a therapist, a forty-year-old psychology student who was the only person who could see me and was covered by my insurance. Unfortunately, she was not very helpful. She put me on the drug Ativan, which made me more jittery, making things worse.
Then in early September I had my quarterly appointment with my oncology GYN surgeon who informed me, after a scan, that I now had a tumor the size of a softball growing on my pelvic floor. I was in a state of shock. When we left his office, there was no social worker or counselor to talk to and no one offered to set us up with one. We were on our own.
Two years earlier I had been diagnosed with stage-one endometrial cancer. After a laparoscopic hysterectomy, my surgeon told me that I had a 99% chance of a complete recovery. I just needed to have a check up every three months for two years, then every six months for another four years.
It never occurred to me that I would be in the 1% category of the operation not working. And I wondered, considering the size of the tumor, if the surgeon had missed it during the last quarterly appointment because he hadn’t had time to do an internal exam. He just did an external palpation and said I was good for another thirty years. So much for managed care.
When we got home after that first appointment, I asked John to call my brother. John went out on the porch and came back in a few minutes to say Gary and his wife Joyce were driving in the car and couldn’t talk, but would try to call back the next day. I could feel the tears rolling down my cheeks, but I refused to cry out loud. I just closed my eyes and lay down on the sofa.
To make matters worse, our dear friend and minister Terry Burke was diagnosed with lung cancer the same week I received my diagnosis. He didn’t even smoke. Both John and I felt heartbroken.
At my next appointment my surgeon told me the tumor was almost attached to my bladder and bowel and that surgery could not be done unless I wanted to have a high-risk procedure called a total pelvic exenteration, which would leave me without a bowel, bladder, or rectum. I would have bags to replace them. The success rate was less than 20% and the infection rate was extremely high, causing the need for other risky surgeries. When John asked our nurse what she would do, she said she wouldn’t do the surgery.
We got a second opinion with the same answer. Instead of my surgeon offering us some emotional and psychological support, especially since I had already been experiencing panic attacks before any of this was known, my husband and I were sent home and told to wait until the surgeon figured out the next moves. For the next two months I lived in fear of the killer inside of me. Every twitch and pain put me into a spin of fear, worry, and anger.
I was angry at the doctors for what felt like their lack of empathy, knowledge, and ability to clearly speak to John and me about what was going on. After all, the hospital and doctors were part of the Harvard Medical Teaching Group and my surgeon was considered by many sources to be one of the top oncologists in Boston and the US.
It took two months to figure out insurance coverage to get a PET scan and for our surgeon to team up with a radiologist and a chemo doctor. For two long months I had little care except for a social worker at the hospital who tried her best to help me but was not reading my panic very well. They finally decided to try radiation and chemotherapy but admitted it probably wouldn’t kill the tumor, just delay the inevitable.
Halfway through the treatment, I had an emotional breakdown during a radiation appointment. Luckily I had John and my friend Rena Pendergast with me. John was so angry he put me in a wheelchair and rolled me into the social worker’s office saying: “Now do you believe Dale needs real psych help?”
Not only was I nosediving because of the terrifying diagnosis, but also because I felt sucker punched by the universe. How could this happen to me? Wasn’t I a good person? Didn’t I have a good relationship with God, and wasn’t I considered one of his helpers? I lived my life with the principles of accountability, compassion, and love. And by the way, hadn’t enough shitty things happened along the way for me to have paid back my karma? Didn’t I do that in spades dealing with Len’s stroke, the dual death of his parents, the heartache I felt as a mom wanting to heal my children who were wounded because I’d been in a bad marriage.
Hadn’t I paid my dues yet?
I felt like Jesus hanging on the cross sputtering, “Father, why have you forsaken me?” What the hell had I done wrong to bring this on myself? I was naïve, I realized: my whole premise for how to live had been coated with the absurd idea that I somehow would avoid any more pain in my life because I had experienced so much already.
But by the time I could finally accept this, I was already falling down the rabbit hole. None of the professionals I had contact with in the Boston medical community knew how to talk to me in a way that would help me understand I was not mentally ill but spiritually broken. I was having a diagnosable experience called a spiritual crisis as explained by Stanislov Grof. I was not losing my mind.
Western culture doesn’t deal well with death; this is especially true of the very professionals who profess that they do. The psychiatrist I was finally assigned to after two months of breaking down and waiting for help was not helpful. She just couldn’t figure out what was causing me to feel so scared and helpless. Had she ever seen a newly diagnosed woman with just a few months to live not break down?
Because they didn’t acknowledge the spiritual nature of being told that I was going to die soon, the psychologists I saw and the doctors and nurses I dealt with were useless. None of them acted knowledgeably or compassionately, except one or two rare people.
During this time and throughout my illness, John was my rock and I relied on his wisdom. He came to every appointment and treatment, often prepared with questions, and fought the bureaucracy and incompetence every step of the way. He eventually fired all our doctors at the hospital and then took me over to the Dana-Farber, where we finally got good care. But sometimes even he would break down and cry during emotional discussions with the doctors, and I knew this was eating him up inside.
I finished treatments just before Christmas 2013 and somehow got through the holidays. But the fear was building up and starting to manifest itself in psychotic behavior, like being afraid we would have to leave our home; unfounded money worries; and distress over even little things, like the heat thermostat being broken.
My family gathered around me, frustrated because nothing they said or did could make me calm down. They called the BEST Team, a group of therapists who visit people’s homes to determine if they need help. After a few visits, they advised me to voluntarily admit myself to the hospital’s psych ward, saying I just needed a few days of round-the-clock comprehensive treatment and I’d be fine.
Needless to say, I didn’t believe them. I thought they were going to throw me into a psych ward with no real plan on how to help me. And I was right.
As the family piled into two cars and turned down Dane Street, I softly said, “Good-bye, neighborhood.” John immediately turned around from the driver’s seat and vowed I would be coming back, and in better shape. That gave me a shot of courage. I’d need it.
The BEST Team assured us everything was all set at the emergency room and I would be processed quickly. It was about 3pm. When we arrived there, most of the family sat down in the waiting lounge while my sister Lynn joined John and me in the medical area. It took a while to get registered, and after an hour or so John asked when the bed in the psych ward would be open. They said soon, so John went back to the lounge to inform the family.
Meanwhile, I saw Lynn talking to a doctor outside my room. I was glad she was there. She’d been through this with her husband a few years earlier.
But when John returned things seemed different. All of a sudden we had a male orderly standing by the door and a new bevy of doctors who came in to interview me. They said it was going to be a while before the bed was ready and they had decided to move me downstairs to open up my current room. When John and I got there, however, something felt wrong. The new room looked more like a holding cell with guards all around.
We’d now been in the ER over five hours and John was pretty mad. But no one could tell us what was going on. John finally told them we were fed up with the wait and were going back home. That’s when we found out I couldn’t leave.
So after nine hours of hell, at midnight, they dragged me away from John. I will never forget the look of despair on his face.
That first night I was in terror. They brought me to a dark dorm room and I lay there thinking I might never get out.
But John went right to work to do just that. He organized visits by all our friends, especially our medical friends, during both the afternoon and evening visiting hours. Adam also came every day. At one point the staff told us 75% of all visitors were mine. Our friend Paul Miller, a psychologist, and our neighbor Dr. Alicia Powell, who came to our aid during my first panic attack, were especially helpful and kept demanding to see my records. The staff kept finding excuses until John finally threatened to hire a lawyer and write an op-ed piece for the Boston Globe. That’s when we finally discovered why my status had changed from voluntary to involuntary Section 12 admittance: that night Lynn had told the ER doctor she thought I might hurt myself.
Meanwhile I was stuck in a locked-down ward, getting no real treatment and falling into more despair. It got so bad I was certain John would come to visit me and I wouldn’t be there. I’d be in some warehouse, unknown, for the rest of my life.
Living in the ward was like being in the movie One Flew Over the Cuckoo’s Nest, complete with the McMurphy and Nurse Ratched characters. But I did start to realize that the safest and most helpful people there were not the doctors or staff, but the other patients who treated me with compassion and taught me how things really worked in the ward. I began to understand some of the stories John had told me about dealing with indigent folks during his twenty years as an inner-city journalist. He always said he admired their courage, honesty, and how they tried to help each other out. Now it was my turn to learn that lesson.
After almost three weeks, the doctors finally responded to all the pressure to let me out and gave me the option of starting electroconvulsive therapy, called ECT, with the agreement I could finish the sessions as an outpatient.
At first I was very hesitant, and Adam was totally against it. We both remembered how hard it was for my mom when she had ECT years before, and I think Adam was afraid it would just scramble my brain and he would lose the real me.
I had inoperable cancer, I was terminally ill. Wouldn’t it be better if the system dealt with the root of the problem and treated me like a person instead of a broken machine?
But I relented, figuring that it was the only way out. The protocol called for seven to twelve sessions. After I had the first one in the clinic downstairs, both John and Adam said they saw a big difference in my demeanor. I don’t know if it was the treatment or the realization this was a path out of there, but I did one more and they let me go.
I came home after three weeks in hell to the cheers and love of our many neighbors and friends. I did two more outpatient ECTs and quit. I knew I didn’t need any more, despite what the doctors had said. Then I settled into what I can only call a period of spiritual limbo.
I watched a lot of bad TV to distract myself. To his credit John joined me most of the time, suffering through Project Runway and The Real Housewives of Beverly Hills, but not without an occasional caustic comment. To just sit on the sofa in his arms made me feel safe for the moment, and I knew that was all we had.
John also helped me organize visits from friends and neighbors literally every day because I needed the feeling of people around me, especially during the daytime. I think this took the place of family since everyone in mine lived out of state, except Adam, who lived in a nearby town and often came over.
In late-winter of 2014 I was surprised to find out John convinced the head of my ministry program, Jyoti, to stop by for a few days on her way back from Europe. I felt both honored and scared. I didn’t want her to see me like this, evading reality by distracting myself.
When she arrived, I was even more surprised to find out she planned to ordain me as a minister right in my home.
“But I haven’t finished reading all the books,” I told her.
She looked at me and smiled. “Oh honey, you don’t have to read more books. You’re writing your own right now.”
We invited our minister Terry, his wife Ellen, our friends Catherine Sasanov and Paul Miller, and Adam to the ceremony. Jyoti wanted to use natural water so John got bundled up, grabbed a hammer and bucket, and headed off to Jamaica Pond at the end of our street. It was really cold and the pond was frozen stiff, but he finally found a place he could break through and returned with the H2O.
John put the bucket on a radiator to warm it up, but it still had a bite to it when Jyoti washed my feet during the ceremony.
Anyway, I finally found a therapist, a forty-year-old psychology student who was the only person who could see me and was covered by my insurance. Unfortunately, she was not very helpful. She put me on the drug Ativan, which made me more jittery, making things worse.
Then in early September I had my quarterly appointment with my oncology GYN surgeon who informed me, after a scan, that I now had a tumor the size of a softball growing on my pelvic floor. I was in a state of shock. When we left his office, there was no social worker or counselor to talk to and no one offered to set us up with one. We were on our own.
Two years earlier I had been diagnosed with stage-one endometrial cancer. After a laparoscopic hysterectomy, my surgeon told me that I had a 99% chance of a complete recovery. I just needed to have a check up every three months for two years, then every six months for another four years.
It never occurred to me that I would be in the 1% category of the operation not working. And I wondered, considering the size of the tumor, if the surgeon had missed it during the last quarterly appointment because he hadn’t had time to do an internal exam. He just did an external palpation and said I was good for another thirty years. So much for managed care.
When we got home after that first appointment, I asked John to call my brother. John went out on the porch and came back in a few minutes to say Gary and his wife Joyce were driving in the car and couldn’t talk, but would try to call back the next day. I could feel the tears rolling down my cheeks, but I refused to cry out loud. I just closed my eyes and lay down on the sofa.
To make matters worse, our dear friend and minister Terry Burke was diagnosed with lung cancer the same week I received my diagnosis. He didn’t even smoke. Both John and I felt heartbroken.
At my next appointment my surgeon told me the tumor was almost attached to my bladder and bowel and that surgery could not be done unless I wanted to have a high-risk procedure called a total pelvic exenteration, which would leave me without a bowel, bladder, or rectum. I would have bags to replace them. The success rate was less than 20% and the infection rate was extremely high, causing the need for other risky surgeries. When John asked our nurse what she would do, she said she wouldn’t do the surgery.
We got a second opinion with the same answer. Instead of my surgeon offering us some emotional and psychological support, especially since I had already been experiencing panic attacks before any of this was known, my husband and I were sent home and told to wait until the surgeon figured out the next moves. For the next two months I lived in fear of the killer inside of me. Every twitch and pain put me into a spin of fear, worry, and anger.
I was angry at the doctors for what felt like their lack of empathy, knowledge, and ability to clearly speak to John and me about what was going on. After all, the hospital and doctors were part of the Harvard Medical Teaching Group and my surgeon was considered by many sources to be one of the top oncologists in Boston and the US.
It took two months to figure out insurance coverage to get a PET scan and for our surgeon to team up with a radiologist and a chemo doctor. For two long months I had little care except for a social worker at the hospital who tried her best to help me but was not reading my panic very well. They finally decided to try radiation and chemotherapy but admitted it probably wouldn’t kill the tumor, just delay the inevitable.
Halfway through the treatment, I had an emotional breakdown during a radiation appointment. Luckily I had John and my friend Rena Pendergast with me. John was so angry he put me in a wheelchair and rolled me into the social worker’s office saying: “Now do you believe Dale needs real psych help?”
Not only was I nosediving because of the terrifying diagnosis, but also because I felt sucker punched by the universe. How could this happen to me? Wasn’t I a good person? Didn’t I have a good relationship with God, and wasn’t I considered one of his helpers? I lived my life with the principles of accountability, compassion, and love. And by the way, hadn’t enough shitty things happened along the way for me to have paid back my karma? Didn’t I do that in spades dealing with Len’s stroke, the dual death of his parents, the heartache I felt as a mom wanting to heal my children who were wounded because I’d been in a bad marriage.
Hadn’t I paid my dues yet?
I felt like Jesus hanging on the cross sputtering, “Father, why have you forsaken me?” What the hell had I done wrong to bring this on myself? I was naïve, I realized: my whole premise for how to live had been coated with the absurd idea that I somehow would avoid any more pain in my life because I had experienced so much already.
But by the time I could finally accept this, I was already falling down the rabbit hole. None of the professionals I had contact with in the Boston medical community knew how to talk to me in a way that would help me understand I was not mentally ill but spiritually broken. I was having a diagnosable experience called a spiritual crisis as explained by Stanislov Grof. I was not losing my mind.
Western culture doesn’t deal well with death; this is especially true of the very professionals who profess that they do. The psychiatrist I was finally assigned to after two months of breaking down and waiting for help was not helpful. She just couldn’t figure out what was causing me to feel so scared and helpless. Had she ever seen a newly diagnosed woman with just a few months to live not break down?
Because they didn’t acknowledge the spiritual nature of being told that I was going to die soon, the psychologists I saw and the doctors and nurses I dealt with were useless. None of them acted knowledgeably or compassionately, except one or two rare people.
During this time and throughout my illness, John was my rock and I relied on his wisdom. He came to every appointment and treatment, often prepared with questions, and fought the bureaucracy and incompetence every step of the way. He eventually fired all our doctors at the hospital and then took me over to the Dana-Farber, where we finally got good care. But sometimes even he would break down and cry during emotional discussions with the doctors, and I knew this was eating him up inside.
I finished treatments just before Christmas 2013 and somehow got through the holidays. But the fear was building up and starting to manifest itself in psychotic behavior, like being afraid we would have to leave our home; unfounded money worries; and distress over even little things, like the heat thermostat being broken.
My family gathered around me, frustrated because nothing they said or did could make me calm down. They called the BEST Team, a group of therapists who visit people’s homes to determine if they need help. After a few visits, they advised me to voluntarily admit myself to the hospital’s psych ward, saying I just needed a few days of round-the-clock comprehensive treatment and I’d be fine.
Needless to say, I didn’t believe them. I thought they were going to throw me into a psych ward with no real plan on how to help me. And I was right.
As the family piled into two cars and turned down Dane Street, I softly said, “Good-bye, neighborhood.” John immediately turned around from the driver’s seat and vowed I would be coming back, and in better shape. That gave me a shot of courage. I’d need it.
The BEST Team assured us everything was all set at the emergency room and I would be processed quickly. It was about 3pm. When we arrived there, most of the family sat down in the waiting lounge while my sister Lynn joined John and me in the medical area. It took a while to get registered, and after an hour or so John asked when the bed in the psych ward would be open. They said soon, so John went back to the lounge to inform the family.
Meanwhile, I saw Lynn talking to a doctor outside my room. I was glad she was there. She’d been through this with her husband a few years earlier.
But when John returned things seemed different. All of a sudden we had a male orderly standing by the door and a new bevy of doctors who came in to interview me. They said it was going to be a while before the bed was ready and they had decided to move me downstairs to open up my current room. When John and I got there, however, something felt wrong. The new room looked more like a holding cell with guards all around.
We’d now been in the ER over five hours and John was pretty mad. But no one could tell us what was going on. John finally told them we were fed up with the wait and were going back home. That’s when we found out I couldn’t leave.
So after nine hours of hell, at midnight, they dragged me away from John. I will never forget the look of despair on his face.
That first night I was in terror. They brought me to a dark dorm room and I lay there thinking I might never get out.
But John went right to work to do just that. He organized visits by all our friends, especially our medical friends, during both the afternoon and evening visiting hours. Adam also came every day. At one point the staff told us 75% of all visitors were mine. Our friend Paul Miller, a psychologist, and our neighbor Dr. Alicia Powell, who came to our aid during my first panic attack, were especially helpful and kept demanding to see my records. The staff kept finding excuses until John finally threatened to hire a lawyer and write an op-ed piece for the Boston Globe. That’s when we finally discovered why my status had changed from voluntary to involuntary Section 12 admittance: that night Lynn had told the ER doctor she thought I might hurt myself.
Meanwhile I was stuck in a locked-down ward, getting no real treatment and falling into more despair. It got so bad I was certain John would come to visit me and I wouldn’t be there. I’d be in some warehouse, unknown, for the rest of my life.
Living in the ward was like being in the movie One Flew Over the Cuckoo’s Nest, complete with the McMurphy and Nurse Ratched characters. But I did start to realize that the safest and most helpful people there were not the doctors or staff, but the other patients who treated me with compassion and taught me how things really worked in the ward. I began to understand some of the stories John had told me about dealing with indigent folks during his twenty years as an inner-city journalist. He always said he admired their courage, honesty, and how they tried to help each other out. Now it was my turn to learn that lesson.
After almost three weeks, the doctors finally responded to all the pressure to let me out and gave me the option of starting electroconvulsive therapy, called ECT, with the agreement I could finish the sessions as an outpatient.
At first I was very hesitant, and Adam was totally against it. We both remembered how hard it was for my mom when she had ECT years before, and I think Adam was afraid it would just scramble my brain and he would lose the real me.
I had inoperable cancer, I was terminally ill. Wouldn’t it be better if the system dealt with the root of the problem and treated me like a person instead of a broken machine?
But I relented, figuring that it was the only way out. The protocol called for seven to twelve sessions. After I had the first one in the clinic downstairs, both John and Adam said they saw a big difference in my demeanor. I don’t know if it was the treatment or the realization this was a path out of there, but I did one more and they let me go.
I came home after three weeks in hell to the cheers and love of our many neighbors and friends. I did two more outpatient ECTs and quit. I knew I didn’t need any more, despite what the doctors had said. Then I settled into what I can only call a period of spiritual limbo.
I watched a lot of bad TV to distract myself. To his credit John joined me most of the time, suffering through Project Runway and The Real Housewives of Beverly Hills, but not without an occasional caustic comment. To just sit on the sofa in his arms made me feel safe for the moment, and I knew that was all we had.
John also helped me organize visits from friends and neighbors literally every day because I needed the feeling of people around me, especially during the daytime. I think this took the place of family since everyone in mine lived out of state, except Adam, who lived in a nearby town and often came over.
In late-winter of 2014 I was surprised to find out John convinced the head of my ministry program, Jyoti, to stop by for a few days on her way back from Europe. I felt both honored and scared. I didn’t want her to see me like this, evading reality by distracting myself.
When she arrived, I was even more surprised to find out she planned to ordain me as a minister right in my home.
“But I haven’t finished reading all the books,” I told her.
She looked at me and smiled. “Oh honey, you don’t have to read more books. You’re writing your own right now.”
We invited our minister Terry, his wife Ellen, our friends Catherine Sasanov and Paul Miller, and Adam to the ceremony. Jyoti wanted to use natural water so John got bundled up, grabbed a hammer and bucket, and headed off to Jamaica Pond at the end of our street. It was really cold and the pond was frozen stiff, but he finally found a place he could break through and returned with the H2O.
John put the bucket on a radiator to warm it up, but it still had a bite to it when Jyoti washed my feet during the ceremony.
 My ordination in our living room 2014
My ordination in our living room 2014 Afterward Terry was the first to congratulate me.
“Welcome to the club, Rev,” he declared as he gave me a big hug.
As time went on Terry and I became very close. He would visit regularly, even when he felt weak or sick from his treatments. We had a simpatico connection only terminally ill people share.
Usually John left us alone while we laughed and cried together in the living room. Terry could swear like a sailor and that always broke me up. And he was very honest about his own fear and anger. He gave me love and courage, even though there was no hope.
Another great helper was my friend Rena, who ministered in a similar nature-based church as the one I belonged to. Rena came to many treatments at the hospital with John and me and visited our home often. Between Rena and Terry I began to reach a spiritual understanding and acceptance that everything is impermanent. I knew every celebration and holiday was probably my last, which made each one a special blessing.
But early in 2015 I had a setback. I hadn’t heard from my sister in quite a while, so I called her. To my surprise she told me she couldn’t visit me anymore because, after dealing with our parents’ and then her husband’s death, she couldn’t endure seeing me die.
My mind understood, but my heart broke. I thought I had always been there for my older sister, and now…
But as John says, if you want to be disappointed ask somebody to do something they can’t or won’t do.
I knew I would never see Lynn again. But I will always love her dearly.
This episode began to bring up a lot of memories, especially of when I was young, and as is the case with many terminally ill people I began to reminisce about my life. How did I get here? What have I done and what have I learned?
I thought back to my family and all the jobs I’ve had. I was a file clerk, a sales clerk, a cashier, a nurse’s aide, a home health aide, a pottery teacher, a journal writing teacher, a poet, twice a real estate agent, an interior designer, and also an entrepreneur who started and ran two home furnishing stores. I was a Reiki Master and Reiki teacher, a sound healer and sound-healing teacher and a minister of the Center for Sacred Studies in California. In between all of this I was also a full-time wife, mother, sister, and friend.
When I thought about my sister Lynn, I remembered how my mother would describe her as “the level-headed one.” My older brother Gary always cracked a joke when my mother said this. He would say, “Mom, ‘level-headed’? Does that mean Lynn has a crew cut?” and then snicker at the image of Lynn with a short flattop hairdo. I imagined a barber with a miniature push mower, mowing Lynn’s level head like a patch of grass.
Lynn was practical and did not take risks or like to try new things. She didn’t like traveling to new places like big cities. She didn’t read the newspaper much, or care too deeply about what was happening in the world, or feel confident driving for six hours alone to visit me in New York or Connecticut. She was the type of person to get a simple, uncomplicated job and never move from it. She didn’t like challenging herself. She was the first to admit this.
As an adult I tried to convince her that she had many talents and abilities that she was very good at. She was trained as a bookkeeper. She would have made a great executive secretary or office manager, but she never wanted to move out of her comfort zone. It irritated me to see someone I loved not using her abilities. It caused some strain between us.
My mother said I was “the restless one,” always searching for something.” It was implied that my searching was not a good quality and that because of it I was flaky and a dilettante. I was perceived as having poor judgment, taking too many risks, and trying too many new things. I made family members feel uncomfortable because I liked change. To me, change felt exhilarating, not something to be afraid of or avoid.
My brother said I took after my father who was also a risk-taker. But my father took risks to become financially successful and I took risks to taste life and see how much I could learn.
After Len had his stroke, I had to learn so many new and challenging things on my own, like how to talk to doctors and find good medical care, how to deal with Len’s business associates and learn when to keep them in the loop and when not to, how to invest and protect our money, and how to emotionally and psychologically support our children as they dealt with an angry disabled parent. Whatever I was afraid to face before his stroke just peeled away under the pressure of what had to be done afterwards.
I became fearless because I had to be. I learned how to embrace change so it wouldn’t destroy me. I learned that taking risks could be experienced as going on an adventure.
Joseph Campbell, the famous mythologist, teacher, and writer, taught that the ancient myths were stories meant to teach us all about life and how to live and view it. By framing life experiences as myths, we can then have a context to put what seem to be random events befalling us into a story that can heal us.
In his book, The Hero with a Thousand Faces, Campbell wrote that if you see yourself as a hero (meaning a common person) going on an adventure (simple life experiences or more complex ones), you “venture forth from the world of common day into a region of supernatural wonder: fabulous forces are there encountered and a decisive victory is won: the hero comes back from this mysterious adventure with the power to bestow boons on his fellow man.”
As my life experiences kept piling up, the more I saw myself as a mythic figure or living a mythic adventure the more I could make sense of things and help myself and others.
When Len had his stroke, I saw myself as Joan of Arc battling the medical and corporate institutions, unable to trust anyone because I learned the hard way that when you have power people play a lot of games to get it from you, either because they want the power or they enjoy watching you lose the power.
I saw myself as young and naïve like Joan of Arc, but full of valor and forthrightness. I was fighting heartless institutions while trying to keep my children safe. I fought for justice and truth, at least in my imagination.
Continued...
“Welcome to the club, Rev,” he declared as he gave me a big hug.
As time went on Terry and I became very close. He would visit regularly, even when he felt weak or sick from his treatments. We had a simpatico connection only terminally ill people share.
Usually John left us alone while we laughed and cried together in the living room. Terry could swear like a sailor and that always broke me up. And he was very honest about his own fear and anger. He gave me love and courage, even though there was no hope.
Another great helper was my friend Rena, who ministered in a similar nature-based church as the one I belonged to. Rena came to many treatments at the hospital with John and me and visited our home often. Between Rena and Terry I began to reach a spiritual understanding and acceptance that everything is impermanent. I knew every celebration and holiday was probably my last, which made each one a special blessing.
But early in 2015 I had a setback. I hadn’t heard from my sister in quite a while, so I called her. To my surprise she told me she couldn’t visit me anymore because, after dealing with our parents’ and then her husband’s death, she couldn’t endure seeing me die.
My mind understood, but my heart broke. I thought I had always been there for my older sister, and now…
But as John says, if you want to be disappointed ask somebody to do something they can’t or won’t do.
I knew I would never see Lynn again. But I will always love her dearly.
This episode began to bring up a lot of memories, especially of when I was young, and as is the case with many terminally ill people I began to reminisce about my life. How did I get here? What have I done and what have I learned?
I thought back to my family and all the jobs I’ve had. I was a file clerk, a sales clerk, a cashier, a nurse’s aide, a home health aide, a pottery teacher, a journal writing teacher, a poet, twice a real estate agent, an interior designer, and also an entrepreneur who started and ran two home furnishing stores. I was a Reiki Master and Reiki teacher, a sound healer and sound-healing teacher and a minister of the Center for Sacred Studies in California. In between all of this I was also a full-time wife, mother, sister, and friend.
When I thought about my sister Lynn, I remembered how my mother would describe her as “the level-headed one.” My older brother Gary always cracked a joke when my mother said this. He would say, “Mom, ‘level-headed’? Does that mean Lynn has a crew cut?” and then snicker at the image of Lynn with a short flattop hairdo. I imagined a barber with a miniature push mower, mowing Lynn’s level head like a patch of grass.
Lynn was practical and did not take risks or like to try new things. She didn’t like traveling to new places like big cities. She didn’t read the newspaper much, or care too deeply about what was happening in the world, or feel confident driving for six hours alone to visit me in New York or Connecticut. She was the type of person to get a simple, uncomplicated job and never move from it. She didn’t like challenging herself. She was the first to admit this.
As an adult I tried to convince her that she had many talents and abilities that she was very good at. She was trained as a bookkeeper. She would have made a great executive secretary or office manager, but she never wanted to move out of her comfort zone. It irritated me to see someone I loved not using her abilities. It caused some strain between us.
My mother said I was “the restless one,” always searching for something.” It was implied that my searching was not a good quality and that because of it I was flaky and a dilettante. I was perceived as having poor judgment, taking too many risks, and trying too many new things. I made family members feel uncomfortable because I liked change. To me, change felt exhilarating, not something to be afraid of or avoid.
My brother said I took after my father who was also a risk-taker. But my father took risks to become financially successful and I took risks to taste life and see how much I could learn.
After Len had his stroke, I had to learn so many new and challenging things on my own, like how to talk to doctors and find good medical care, how to deal with Len’s business associates and learn when to keep them in the loop and when not to, how to invest and protect our money, and how to emotionally and psychologically support our children as they dealt with an angry disabled parent. Whatever I was afraid to face before his stroke just peeled away under the pressure of what had to be done afterwards.
I became fearless because I had to be. I learned how to embrace change so it wouldn’t destroy me. I learned that taking risks could be experienced as going on an adventure.
Joseph Campbell, the famous mythologist, teacher, and writer, taught that the ancient myths were stories meant to teach us all about life and how to live and view it. By framing life experiences as myths, we can then have a context to put what seem to be random events befalling us into a story that can heal us.
In his book, The Hero with a Thousand Faces, Campbell wrote that if you see yourself as a hero (meaning a common person) going on an adventure (simple life experiences or more complex ones), you “venture forth from the world of common day into a region of supernatural wonder: fabulous forces are there encountered and a decisive victory is won: the hero comes back from this mysterious adventure with the power to bestow boons on his fellow man.”
As my life experiences kept piling up, the more I saw myself as a mythic figure or living a mythic adventure the more I could make sense of things and help myself and others.
When Len had his stroke, I saw myself as Joan of Arc battling the medical and corporate institutions, unable to trust anyone because I learned the hard way that when you have power people play a lot of games to get it from you, either because they want the power or they enjoy watching you lose the power.
I saw myself as young and naïve like Joan of Arc, but full of valor and forthrightness. I was fighting heartless institutions while trying to keep my children safe. I fought for justice and truth, at least in my imagination.
Continued...
Editor's Note
by John Swan
After three months of working on her memoir, Dale had to stop writing. The chemotherapy, radiation, drugs and the tumor itself had taken their toll, and she became exhausted.
But writing this memoir was a very healing process for both of us. Back in the fall of 2014, when it was evident that Dale didn’t have much time left, we struggled with the sadness of letting go. Then one day in December 2014 she woke up with an epiphany after a Reiki session from a colleague.
“It was wild,” she said. This phrase kept running through my mind: “My life is compost!”
Being the writer she is, Dale cast that hook out into the universe then sat down on the sofa and over the next three months reeled in this 70,000-word memoir. Every morning I would come downstairs to see her face beaming over her laptop. Our life changed, and we began to enjoy each day one at a time. We learned that the simple things in life are often the most important: the smile you give your lover, holding hands, the laugh of a friend and the smell of a dinner shared with love, our grandsons’ eyes that will someday look deep into the future and hopefully appreciate the past.
Dale asked me to finish her book, and I will do my best, in my own words.
This memoir is her gift “bestowed” to all of us, and a tribute to the love and courage of this amazing woman. She will always be my Sweetheart.
But writing this memoir was a very healing process for both of us. Back in the fall of 2014, when it was evident that Dale didn’t have much time left, we struggled with the sadness of letting go. Then one day in December 2014 she woke up with an epiphany after a Reiki session from a colleague.
“It was wild,” she said. This phrase kept running through my mind: “My life is compost!”
Being the writer she is, Dale cast that hook out into the universe then sat down on the sofa and over the next three months reeled in this 70,000-word memoir. Every morning I would come downstairs to see her face beaming over her laptop. Our life changed, and we began to enjoy each day one at a time. We learned that the simple things in life are often the most important: the smile you give your lover, holding hands, the laugh of a friend and the smell of a dinner shared with love, our grandsons’ eyes that will someday look deep into the future and hopefully appreciate the past.
Dale asked me to finish her book, and I will do my best, in my own words.
This memoir is her gift “bestowed” to all of us, and a tribute to the love and courage of this amazing woman. She will always be my Sweetheart.
Chapter 18 - Conclusion
by John Swan
We had the last appointment with our doctors at Dana-Farber late in the winter of 2015. It was a tough one. We were there to talk about how Dale would die.
Everyone had misty eyes or tears as our oncologist Alexi Wright and palliative care doctor John Halporn gave us the two options. Dale could stop treatment and basically bleed out, or get transfusions so she would last a little longer and let the tumor kill her.
They said bleeding out would be a lot less painful than dying from the tumor eating her bowels and bladder, and they seemed to lean towards the first option but didn’t really try to persuade us. Then we talked about bringing in hospice services right now so they could get to know us and what we needed.
It was a profound moment. As I held Dale’s hand it finally hit me: she’s really going to die—I’m going to lose her. Up until that moment I had stayed hyperfocused on the next step of this journey, partly so I didn’t have to dwell on what was ahead. But now we were approaching the last step.
Dale was probably the calmest of us all. She asked some questions and nodded that she understood what they said.
At the end of the appointment, Dale thanked them for their kindness and they both gave her a hug. “I’ll let you know what I decide,” she told them. But I already thought I knew her decision.
When we got home Dale sat on the sofa and didn’t say a word. I gave her some time to be alone, then came in and sat down beside her. We held each other and cried, mostly me. She wiped my tears with her palms and gave me a kiss.
“I’m going with the first option,” she said.
“I thought so. Can we talk about it?”
“Not now. Later, okay?”
That evening Dale explained that she was afraid of all the pain from the tumor and would like to go softly into the night. I knew she had researched assisted suicide on the Internet, but she didn’t talk about it much.
“Can I tell you what I’d do?” I asked. She nodded. “I’d get the transfusions, stay as strong as I can for as long as I can, and when the tumor gets too bad take the black pill.”
“I don’t know if I could do that. I really don’t. The other way seems more like letting nature take its course.”
For a few days both Adam and I gently tried to convince Dale to change her mind, to no avail. She had made her decision. So it would be.
I called a highly recommended hospice group and set up an interview with their rep at our home. It went well. We were assured we would “get the care we needed, when we needed it.” So we signed up. At first we just had a nurse come once a week and get to know us.
In early March Joel and his girlfriend Liz visited us. Dale adored Liz and considered her a daughter. She was down-to-earth, loving, and a good partner for Joel.
Dale was determined to have one last family outing. Of course she chose the Museum of Fine Arts, one of her favorite places to hang out. Dale loved museums, I think because they’re the home of the muses and inspiration. And she hoped some of that might rub off on her family.
The winter of ‘15 was brutal, often with four feet of snow on the ground. By March the snow still clogged the city streets and parking places.
Adam joined us and we all drove through the muck to the MFA side parking garage. I offered to first drop Dale off at the entrance, but she wanted to walk all the way around to the front of this huge building. She was obviously struggling.
We got inside and I pleaded with Dale to take one of the many wheelchairs available. She declined, saying she would be okay. We would just rest when she needed to, and we could keep tabs on the kids by cell phone.
Dale could be very stubborn, and I usually loved that about her. But in this case it turned out to be a bad decision. I should have said more or even demanded she use a wheel.chair, but in the larger picture I knew I had to also let her try and fail, just like I knew I had to let her die.
Everyone went their own way, but soon Dale needed to sit down. All of a sudden she wasn’t feeling well. I called the kids and they joined us in the lobby. A very kind attendant brought us a wheelchair and I brought the car around back, picked her up, and we went home in silence.
A few days later Dale jumped off the sofa to rush to the bathroom. With all her weight leaning forward, her feet couldn’t stop her and she crashed into the kitchen door jam. Stunned but okay, she sat up on the floor and I got some ice to put on her forehead.
“They’re going to think you beat me up,” she laughed feeling the bump with her hand.
Then she began to cry. All I could do was hold her.
After that Dale started to use a cane. Soon she needed a walker. She hated it. She was losing control of the simplest things and declining every day.
About this time we began to have some problems with hospice. I noticed our nurse seemed confused sometimes about things like counting meds and giving me instructions on Dale’s care. I confronted her about this and she got indignant, reminding me she was a professional with a lot of experience. I began to have doubts about the group, thinking we’d been through this before with many of our first doctors.
In mid-April Joel and Adam moved in with us. They were a great help, and I realized how much I had missed family support during the past twenty months.
I also started editing the first edition of Dale’s memoir with the goal of getting it self-published and in her hands before she died. I did the first pass edits then sent chapters out to my writing friends who completed their edits in just a few days.
Caitlin Bechtel at the Harvard Bookstore put us at the head of the queue. Working together we designed the front and back covers, and then she did the formatting during the weekend. By Wednesday we had a box of copies that Adam picked up and brought home to the cheers of friends who were visiting that day. I’ll never forget the smile on Dale’s face as I handed her the first copy. She was exhausted from her illness, but amazed she was holding the book that she had always dreamed of writing. The whole process took about two weeks and must have been a record turnaround for the publisher.
Dale’s niece, Kelly Powell, also began formatting the first edition for Dale’s new blog, daleswan.weebly.com. She had it up and running within a week. Kelly had been a great help throughout Dale’s illness, visiting several times despite her stressful business and family obligations. Dale loved Kelly very much and was in many ways Kelly’s surrogate mom.
During this time Dale’s many friends, colleagues and students continued to visit her every day, as they had for the past twenty months—over forty people altogether. A smaller group seemed to be there constantly, including friends Steve Quann and Diana Satin, Catherine Sasanov and Paul Miller, Beth Mahar, Rena Pendergast, Karen D’Amato, and Dale’s colleague Lisa Biagetti, who gave Dale weekly Reiki sessions. And of course there was our minister Terry, who was not doing great himself, and especially Dale’s closest friend and a true sister Renée DeKona. They were all unbelievable and I will never forget their kindness.
Soon Dale was having so much trouble using the stairs that Joel and Adam moved our bed downstairs to my study, which was under our bedroom and next to the downstairs bathroom. I was happy to see them working together and hopefully starting to appreciate each other after years of silence between them.
Dale decided she wanted some of her ashes buried under Beth’s beautiful sugar maple tree close to our house. It was the first thing she saw each morning through the window when she got out of bed. Beth and Kevin, two kind souls, agreed.
She also wanted some ashes spread among a stand of trees on the Eastern Promenade in Portland, Maine. Portland was where she’d first really struck out on her own, and she’d spent many hours walking her dog Zoe on the Prom.
The rest of her ashes she wanted combined with mine when I die and buried under Beth’s maple tree “so we’ll be together forever, in our neighborhood,” she said.
Dale also came up with the idea of creating a foundation to teach therapeutic writing to critically ill patients and their families. Those plans are going ahead with the formation of a board of directors.
We continued to have problems with hospice: home health aides were not showing up, our nurse’s combative attitude continued, and we had no comprehensive coverage. So I hired a private home health aide from 2pm to 10pm. to augment the thin hospice coverage. Even then I had to get up twice each night to change Dale’s diapers, a task I wasn’t very good at and one that embarrassed Dale.
Then one morning I woke up to an empty bed. Where’s Dale? I leaned over to find her crumpled on the floor beside the bed. I got her back in and immediately called hospice, saying my wife had fallen out of bed, may have been injured, and needed a nurse right away.
I couldn’t call 911 because I was told by hospice that they would take her to the hospital and she’d never get out.
No nurse came. I called hospice again, and again. By early afternoon I called Dr. Halporn at Dana-Farber and explained the situation. He said he finished rounds at 5 and would be at our house by 5:30pm.
And he was. No hospice nurse ever showed up or called. The doctor checked Dale out then stayed and talked to us for over an hour.
The next day, a Saturday, Dale’s psychiatrist from Dana-Farber, Fremonta Meyer, took the subway crosstown to visit us on her day off. It was obvious the doctors at Dana-Farber really cared about Dale and saw her as an extraordinary woman.
Meanwhile, Joel, Adam, and I were seething about the lack of hospice care. I called a supervisor, complaining for an hour as I got the runaround. Then I mentioned I was a journalist and maybe my best option now was to write an op-ed piece for the newspapers about their group.
Within forty-five minutes I got a call from the medical director offering to meet at our home. When she got there I laid it all out for her and she admitted, “That’s unacceptable.”
“And just what does that mean?” I asked.
She then offered round-the-clock coverage starting that night.
Finally, in her last days, Dale received the hospice care they had promised.
But the death process itself was much different than the sanitized version we were told at Dana-Farber. Dale was actually starving, bleeding, and suffocating to death. All they could do was increase the drugs, especially the morphine.
As they did, Dale had fewer and fewer conscious moments. They finally became just little windows of time between doses. She would ask me questions during these times, and I tried to answer honestly but with composure so my grief wouldn’t scare her. But the tears came anyway. I couldn’t stop them. I was running on fumes and teetering on the edge of losing it.
“Will I walk again?”
“No, sweetie, you won’t.
“Am I dying?”
“Yes. But I’m here with you. I’ll always be with you, forever.”
“What did I do wrong?”
“Oh sweetie, you didn’t do anything wrong. You are the best person I’ve ever known. You did nothing wrong.”
On the morning of her last day, Dale started calling for her sister. What could I say?
“The kids are here for you, darling. So are your friends.”
Then in the afternoon she opened her eyes and took my hand. “Don’t forget me,” she pleaded.
I came very close to breaking down. “Oh baby, how could I ever forget you? You are the most amazing miracle in my life. You will always be right here,” I said tapping my heart.
Later that evening Dale came to for the last time. She struggled to say something and I leaned over and put my ear to her lips. “I love you,” she told me in the quietest voice I’d ever heard.
“And I will always love you,” I told her with tears streaming down my face. We had said our good-byes.
A few hours later in the early morning of April 26, 2015, with her boys by her side, my beautiful Sweetheart, the light of my life, died in my arms in her own bed, in our home in Jamaica Plain. It was her final wish.
Everyone had misty eyes or tears as our oncologist Alexi Wright and palliative care doctor John Halporn gave us the two options. Dale could stop treatment and basically bleed out, or get transfusions so she would last a little longer and let the tumor kill her.
They said bleeding out would be a lot less painful than dying from the tumor eating her bowels and bladder, and they seemed to lean towards the first option but didn’t really try to persuade us. Then we talked about bringing in hospice services right now so they could get to know us and what we needed.
It was a profound moment. As I held Dale’s hand it finally hit me: she’s really going to die—I’m going to lose her. Up until that moment I had stayed hyperfocused on the next step of this journey, partly so I didn’t have to dwell on what was ahead. But now we were approaching the last step.
Dale was probably the calmest of us all. She asked some questions and nodded that she understood what they said.
At the end of the appointment, Dale thanked them for their kindness and they both gave her a hug. “I’ll let you know what I decide,” she told them. But I already thought I knew her decision.
When we got home Dale sat on the sofa and didn’t say a word. I gave her some time to be alone, then came in and sat down beside her. We held each other and cried, mostly me. She wiped my tears with her palms and gave me a kiss.
“I’m going with the first option,” she said.
“I thought so. Can we talk about it?”
“Not now. Later, okay?”
That evening Dale explained that she was afraid of all the pain from the tumor and would like to go softly into the night. I knew she had researched assisted suicide on the Internet, but she didn’t talk about it much.
“Can I tell you what I’d do?” I asked. She nodded. “I’d get the transfusions, stay as strong as I can for as long as I can, and when the tumor gets too bad take the black pill.”
“I don’t know if I could do that. I really don’t. The other way seems more like letting nature take its course.”
For a few days both Adam and I gently tried to convince Dale to change her mind, to no avail. She had made her decision. So it would be.
I called a highly recommended hospice group and set up an interview with their rep at our home. It went well. We were assured we would “get the care we needed, when we needed it.” So we signed up. At first we just had a nurse come once a week and get to know us.
In early March Joel and his girlfriend Liz visited us. Dale adored Liz and considered her a daughter. She was down-to-earth, loving, and a good partner for Joel.
Dale was determined to have one last family outing. Of course she chose the Museum of Fine Arts, one of her favorite places to hang out. Dale loved museums, I think because they’re the home of the muses and inspiration. And she hoped some of that might rub off on her family.
The winter of ‘15 was brutal, often with four feet of snow on the ground. By March the snow still clogged the city streets and parking places.
Adam joined us and we all drove through the muck to the MFA side parking garage. I offered to first drop Dale off at the entrance, but she wanted to walk all the way around to the front of this huge building. She was obviously struggling.
We got inside and I pleaded with Dale to take one of the many wheelchairs available. She declined, saying she would be okay. We would just rest when she needed to, and we could keep tabs on the kids by cell phone.
Dale could be very stubborn, and I usually loved that about her. But in this case it turned out to be a bad decision. I should have said more or even demanded she use a wheel.chair, but in the larger picture I knew I had to also let her try and fail, just like I knew I had to let her die.
Everyone went their own way, but soon Dale needed to sit down. All of a sudden she wasn’t feeling well. I called the kids and they joined us in the lobby. A very kind attendant brought us a wheelchair and I brought the car around back, picked her up, and we went home in silence.
A few days later Dale jumped off the sofa to rush to the bathroom. With all her weight leaning forward, her feet couldn’t stop her and she crashed into the kitchen door jam. Stunned but okay, she sat up on the floor and I got some ice to put on her forehead.
“They’re going to think you beat me up,” she laughed feeling the bump with her hand.
Then she began to cry. All I could do was hold her.
After that Dale started to use a cane. Soon she needed a walker. She hated it. She was losing control of the simplest things and declining every day.
About this time we began to have some problems with hospice. I noticed our nurse seemed confused sometimes about things like counting meds and giving me instructions on Dale’s care. I confronted her about this and she got indignant, reminding me she was a professional with a lot of experience. I began to have doubts about the group, thinking we’d been through this before with many of our first doctors.
In mid-April Joel and Adam moved in with us. They were a great help, and I realized how much I had missed family support during the past twenty months.
I also started editing the first edition of Dale’s memoir with the goal of getting it self-published and in her hands before she died. I did the first pass edits then sent chapters out to my writing friends who completed their edits in just a few days.
Caitlin Bechtel at the Harvard Bookstore put us at the head of the queue. Working together we designed the front and back covers, and then she did the formatting during the weekend. By Wednesday we had a box of copies that Adam picked up and brought home to the cheers of friends who were visiting that day. I’ll never forget the smile on Dale’s face as I handed her the first copy. She was exhausted from her illness, but amazed she was holding the book that she had always dreamed of writing. The whole process took about two weeks and must have been a record turnaround for the publisher.
Dale’s niece, Kelly Powell, also began formatting the first edition for Dale’s new blog, daleswan.weebly.com. She had it up and running within a week. Kelly had been a great help throughout Dale’s illness, visiting several times despite her stressful business and family obligations. Dale loved Kelly very much and was in many ways Kelly’s surrogate mom.
During this time Dale’s many friends, colleagues and students continued to visit her every day, as they had for the past twenty months—over forty people altogether. A smaller group seemed to be there constantly, including friends Steve Quann and Diana Satin, Catherine Sasanov and Paul Miller, Beth Mahar, Rena Pendergast, Karen D’Amato, and Dale’s colleague Lisa Biagetti, who gave Dale weekly Reiki sessions. And of course there was our minister Terry, who was not doing great himself, and especially Dale’s closest friend and a true sister Renée DeKona. They were all unbelievable and I will never forget their kindness.
Soon Dale was having so much trouble using the stairs that Joel and Adam moved our bed downstairs to my study, which was under our bedroom and next to the downstairs bathroom. I was happy to see them working together and hopefully starting to appreciate each other after years of silence between them.
Dale decided she wanted some of her ashes buried under Beth’s beautiful sugar maple tree close to our house. It was the first thing she saw each morning through the window when she got out of bed. Beth and Kevin, two kind souls, agreed.
She also wanted some ashes spread among a stand of trees on the Eastern Promenade in Portland, Maine. Portland was where she’d first really struck out on her own, and she’d spent many hours walking her dog Zoe on the Prom.
The rest of her ashes she wanted combined with mine when I die and buried under Beth’s maple tree “so we’ll be together forever, in our neighborhood,” she said.
Dale also came up with the idea of creating a foundation to teach therapeutic writing to critically ill patients and their families. Those plans are going ahead with the formation of a board of directors.
We continued to have problems with hospice: home health aides were not showing up, our nurse’s combative attitude continued, and we had no comprehensive coverage. So I hired a private home health aide from 2pm to 10pm. to augment the thin hospice coverage. Even then I had to get up twice each night to change Dale’s diapers, a task I wasn’t very good at and one that embarrassed Dale.
Then one morning I woke up to an empty bed. Where’s Dale? I leaned over to find her crumpled on the floor beside the bed. I got her back in and immediately called hospice, saying my wife had fallen out of bed, may have been injured, and needed a nurse right away.
I couldn’t call 911 because I was told by hospice that they would take her to the hospital and she’d never get out.
No nurse came. I called hospice again, and again. By early afternoon I called Dr. Halporn at Dana-Farber and explained the situation. He said he finished rounds at 5 and would be at our house by 5:30pm.
And he was. No hospice nurse ever showed up or called. The doctor checked Dale out then stayed and talked to us for over an hour.
The next day, a Saturday, Dale’s psychiatrist from Dana-Farber, Fremonta Meyer, took the subway crosstown to visit us on her day off. It was obvious the doctors at Dana-Farber really cared about Dale and saw her as an extraordinary woman.
Meanwhile, Joel, Adam, and I were seething about the lack of hospice care. I called a supervisor, complaining for an hour as I got the runaround. Then I mentioned I was a journalist and maybe my best option now was to write an op-ed piece for the newspapers about their group.
Within forty-five minutes I got a call from the medical director offering to meet at our home. When she got there I laid it all out for her and she admitted, “That’s unacceptable.”
“And just what does that mean?” I asked.
She then offered round-the-clock coverage starting that night.
Finally, in her last days, Dale received the hospice care they had promised.
But the death process itself was much different than the sanitized version we were told at Dana-Farber. Dale was actually starving, bleeding, and suffocating to death. All they could do was increase the drugs, especially the morphine.
As they did, Dale had fewer and fewer conscious moments. They finally became just little windows of time between doses. She would ask me questions during these times, and I tried to answer honestly but with composure so my grief wouldn’t scare her. But the tears came anyway. I couldn’t stop them. I was running on fumes and teetering on the edge of losing it.
“Will I walk again?”
“No, sweetie, you won’t.
“Am I dying?”
“Yes. But I’m here with you. I’ll always be with you, forever.”
“What did I do wrong?”
“Oh sweetie, you didn’t do anything wrong. You are the best person I’ve ever known. You did nothing wrong.”
On the morning of her last day, Dale started calling for her sister. What could I say?
“The kids are here for you, darling. So are your friends.”
Then in the afternoon she opened her eyes and took my hand. “Don’t forget me,” she pleaded.
I came very close to breaking down. “Oh baby, how could I ever forget you? You are the most amazing miracle in my life. You will always be right here,” I said tapping my heart.
Later that evening Dale came to for the last time. She struggled to say something and I leaned over and put my ear to her lips. “I love you,” she told me in the quietest voice I’d ever heard.
“And I will always love you,” I told her with tears streaming down my face. We had said our good-byes.
A few hours later in the early morning of April 26, 2015, with her boys by her side, my beautiful Sweetheart, the light of my life, died in my arms in her own bed, in our home in Jamaica Plain. It was her final wish.

